Care Coordination Software: Key to Unlocking Value-Based Care for Providers and Payers
Value-based care continues to reshape how healthcare organisations, ACOs, and payers deliver and manage care. As reimbursement shifts from volume to outcomes, effective coordination becomes essential.
A modern care coordination software platform centralizes patient information, connects multi-disciplinary teams, supports care transitions, and helps both providers and payers improve measurable outcomes.
This article explains why care coordination is central to value-based care, how care coordination platforms reduce clinical and operational friction, and what challenges organisations face when implementing them. The updated structure combines challenges with corresponding solutions to provide actionable clarity for leaders.
Additionally, we explain why a custom-built care coordination solution is often the most reliable and scalable option, especially for hospitals, ACOs, and insurers with unique workflows. As a company experienced in hospital management software development, custom care management, and care management technologies, we describe how our discovery-driven and outcomes-based approach supports your shift to value-based care.
Why Care Coordination Software Matters
Real-time visibility across care settings
Multi-disciplinary teams gain immediate access to patient history, care plans, utilization pattern,s and social factors, allowing them to respond earlier and avoid costly complications.
Efficient workflow automation
Automated tasks — referrals, follow-ups, appointment scheduling, documentation — reduce time spent on manual coordination.
Fewer gaps in care
A shared digital care plan reduces duplication and ensures nothing falls through during transitions (hospital → home, specialist → primary care, etc.).
Better reporting for value-based contracts
Dashboards and analytics help organisations track risk scores, utilization, readmissions, quality metrics, and contract benchmarks.
Member and patient engagement
Better coordination improves adherence, communication, and satisfaction, which are now key performance indicators for payers and ACOs.
Benefits of Care Coordination Software
- Manages chronic conditions through structured care pathways
- Supports remote patient monitoring programs
- Aligns payer-provider workflows
- Reduces readmissions and unnecessary utilization
- Improves adherence and preventive care activities
- Strengthens collaboration across the community and social care
- Supports compliance and audit readiness
- Enables more predictable performance in value-based contracts
All these outcomes become easier with a purpose-built care coordination platform connected to your EHRs, claims systems, labs, telehealth tools, and community care services.
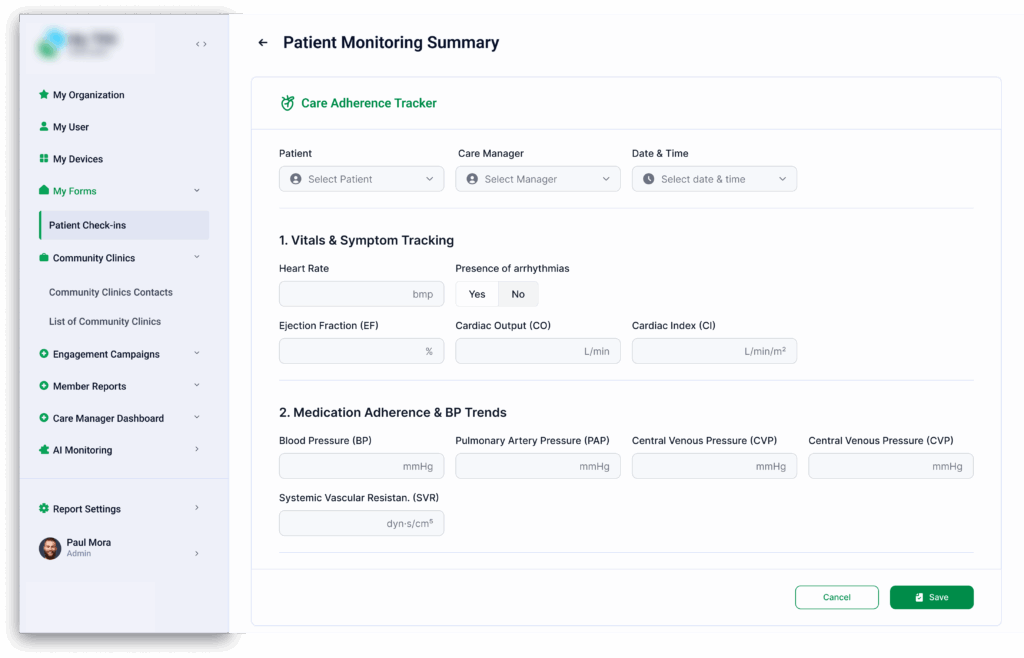
Read about our service: Remote Patient Monitoring Software for Value-Based Care
Challenges in Adopting Care Coordination Software and How to Address Them
Healthcare organisations and payers often recognize the need for stronger coordination, yet implementation is rarely straightforward. Below are the key challenges commonly seen in value-based models, paired with solutions that reflect practical industry experience.
Challenge 1: Fragmented Health IT Ecosystems
Most care teams operate within a landscape of multiple EHRs, claims systems, telehealth tools, and community resource platforms. These systems store data differently, update at different intervals, and often do not communicate efficiently. As a result, teams lose time reconciling information and patients receive inconsistent follow-up.
Solution: Interoperability Standards and Flexible Integration Layers
Interoperability remains the foundation of effective care coordination software. Organisations benefit when they adopt systems built to work with established standards such as HL7 and FHIR.
A flexible integration layer allows your care coordination platform to connect with EHRs, HIEs, payer databases, and social care tools without forcing a complete infrastructure overhaul.
The overarching goal is a unified, accurate patient view that supports both clinical and non-clinical workflows.
Challenge 2: Coordination Across Multiple Settings of Care
Coordination often breaks down during transitions between primary care, specialists, behavioral health providers, post-acute facilities, and community services. Each setting has its own procedures and documentation requirements, leading to miscommunication and delays.
Solution: Workflow Mapping Based on Real-World Processes
Before adopting any care coordination solution, teams benefit from clarifying how referrals, transitions, and follow-ups currently work. Mapping existing pathways helps identify bottlenecks, missing data point,s and duplicated effort.
When workflows are reflected faithfully in the platform, care teams experience less friction. This increases adoption and ensures the technology complements, rather than disrupts, day-to-day operations.
Challenge 3: Heavy Administrative Burden
Manual follow-up calls, referral tracking, documentation, scheduling, and quality reporting often overwhelm nurses, care managers, and administrative staff. This strain reduces time available for direct patient engagement.
Solution: Gradual Automation of Routine Tasks
Automation within care coordination in healthcare does not need to happen all at once. A phased approach is often more effective.
Start by automating predictable, repetitive tasks like appointment reminders, referral status updates, task routing, and data validation.
Removing administrative burden step by step helps teams adapt comfortably while improving consistency and timeliness.
Challenge 4: Data Privacy and Compliance
Sharing information across providers, payers, and community organisations increases exposure to privacy risks. Compliance becomes more complex when social determinants data and home-based care information enter the picture.
Solution: Clear Access Policies and Built-In Compliance Controls
Effective care management technologies include role-based access, audit trails, consent management, and encryption by default.
What matters most is establishing governance rules that determine who can access what information, under which circumstances, and with what level of granularity. Technology should reinforce these policies, not replace them.
Challenge 5: Measuring Performance in Value-Based Care
Many organisations struggle to translate their coordination efforts into measurable outcomes. Without strong reporting tools, it becomes difficult to track improvements in readmissions, chronic disease management, emergency utilization, or contract performance.
Solution: Metrics That Reflect Real Care Delivery
To evaluate a care coordination platform, leaders benefit from selecting metrics tied directly to operational realities. These may include closed-loop referrals, follow-up adherence, SDoH resolution rate,s or care plan progression.
Embedding analytics into daily workflows ensures that insights are continuously available, not generated only at the end of reporting cycles.
Challenge 6: Financial and Resource Limitations
Even when leadership supports coordinated care, teams may struggle with limited budgets, limited IT resources or competing priorities.
Solution: Phased Implementation and Outcome-Based Roadmaps
Instead of large, one-time projects, many organisations prefer incremental rollouts. Start by improving coordination for a specific patient group, such as high-risk chronic patients or those transitioning from hospital to home.
This approach reduces upfront effort, prevents staff overload and allows the organisation to learn what works before expanding.
Challenge 7: Integrating Medical and Social Care
A large portion of preventable utilization is linked to social determinants of health. Yet social care providers often lack connectivity to clinical systems. This breaks the chain of coordination and makes follow-up inconsistent.
Solution: Shared Pathways for Clinical and Social Partners
A practical approach is to build or configure custom care management workflows that include both clinical tasks and social referrals.
By embedding SDoH assessments, community referrals and outcome tracking, organisations ensure that social needs are fully integrated into the care plan.
Challenge 8: Evolving Requirements in Value-Based Programs
ACOs, payers and state programs frequently introduce new requirements. Off-the-shelf systems can struggle to keep up, especially when organisations provide specialized services or operate across multiple regions.
Solution: Configurable Architecture and Adaptable Tools
To stay compliant with changing models, teams benefit from technology that can be adapted through configuration rather than expensive rebuilds.
Experienced care management software vendors focus on flexibility, allowing organisations to adjust rules, workflows and reporting criteria as programs evolve.
This adaptability is particularly important in hospital management software development and population health initiatives, where requirements shift over time.
Why Choose Sigma Software for Care Coordination Software Development
At our company, we combine deep domain experience in value-based care with proven custom software development practices. Here is how we deliver:
- Discovery and Workflow Mapping: We start with a discovery phase — understanding your care pathways, payer-provider or ACO contracts, chronic care and post-acute workflows, referral networks, social care, and community integration.
- Outcome-Driven Design: We prioritize measurable outcomes: lower readmissions, better chronic care control, improved preventive care, lower cost of care, and higher patient/member satisfaction. We build KPIs and reporting dashboards from day one.
- Interoperability & Integration: Using open standards and APIs (FHIR / HL7 or other), we ensure seamless integration with your EHRs, HIEs, lab systems, telehealth platforms, and third-party services (e.g., community referrals).
- Security & Compliance: We embed data privacy, consent management, role-based access, encryption, audit trails, and adherence to relevant regulations (local or international), from the ground up.
- Scalable Architecture & Flexibility: As your organization grows or evolves — e.g., adding remote monitoring, behavioral health, home-care, or new contracts — our platforms scale and adapt without disruptive IT overhauls.
- Agile Delivery & Iteration: We deliver in phases (MVP, pilot, full roll-out), incorporate clinician feedback, and iterate to refine workflows, performance, and user experience.
In short, we don’t deliver generic software. We deliver a custom care coordination solution built around your reality, aligned with value-based care goals, and designed to deliver measurable results.
Practical Checklist for Healthcare Organisations
If you are considering implementing a care coordination platform or building a custom solution, use this checklist to guide your evaluation and planning:
Step/Question | What to Verify / Do |
Define Use Cases & Scope | Map the care pathways you need: chronic disease management, transitional care, post-acute care, behavioral health, social care, remote monitoring, referrals, etc. |
Identify Stakeholders | Include all care team roles: PCPs, specialists, care managers, social workers, payers, and community partners. Determine who needs access to what data. |
Assess Existing IT Landscape | Inventory your current EHRs, lab systems, post-acute systems, telehealth platforms, and community care systems. Look for interoperability gaps. |
Define KPIs & Metrics | Choose measurable outcomes: readmission rate, follow-up time, referral completion, chronic disease control, cost per patient, and utilization measures. |
Security & Compliance Requirements | Determine regulatory obligations (privacy, consent, data sharing), access controls, audit trails, and encryption. |
Decide Between Off-the-Shelf vs Custom | Evaluate whether existing platforms meet your workflows or whether custom development is needed for true alignment. |
Plan Phased Implementation | Start with a pilot or MVP targeting critical care pathways. Collect feedback from clinicians, care teams, and payers. |
Ensure Integration & Interoperability | Use standards (APIs, FHIR/HL7) or build custom interfaces to connect with EHRs, HIEs, labs, and community services. |
Enable Reporting & Analytics | Build dashboards for operational and clinical KPIs. Enable risk stratification, predictive alerts, and utilization tracking. |
Train Users & Manage Change | Provide training for clinicians, care managers, and administrative staff. Ensure workflows are adopted properly. |
Plan for Scale & Evolution | Ensure the platform can grow with your organisation — adding new services like remote monitoring, behavioral health, and member engagement. |
Final thoughts
For healthcare organisations, ACOs, insurers, and payers operating in value-based care models, care coordination software is not a “nice-to-have.” It is foundational. Without robust coordination, data sharing, and integrated care management, fragmented workflows and disconnected systems undermine quality, inflate costs, and impede performance.
Custom-developed solutions offer the flexibility, interoperability, security, and outcome-focused design needed to navigate complex payer-provider relationships, multifaceted care pathways, and evolving value-based contracts.
If you want to move toward value-based care with confidence, consider a tailored care coordination platform as a strategic investment that pays off in improved outcomes, lower costs, and better patient and member experience.
Want to see what this looks like in practice? Let’s talk.
Improved care coordination, lower total cost of care through fewer redundant procedures, better chronic disease control, reduced readmissions, enhanced outcomes, efficient resource utilisation, and improved member experience — enabling organisations to meet VBC contract goals.
Challenges include integrating with legacy IT systems, managing data privacy and compliance, aligning multiple stakeholders across care settings, training staff, and justifying upfront investment without clear ROI.
By embedding encryption (in transit and at rest), role-based access control, audit logs, consent management, configurable data-sharing agreements, and compliance frameworks from the ground up — reducing risk and ensuring adherence to regulatory standards.
Ready to Solve Your Value-Based Care Challenge?
Let’s talk about your unique workflows and design a custom digital health solution that supports outcome-based care, improves population health, and aligns with value-based reimbursement models.
Whether you’re navigating HEDIS metrics, improving care coordination, or optimizing performance-based contracts, we can help.
Build Your Custom Implementation Plan
Your implementation plan includes integrations, MVP timelines, and long-term support strategies. We build your value-based care solution around real workflows, compliance requirements, and measurable outcome goals.
Launch and Optimize for Outcome-Based Development
Our solutions combine predictive analytics, AI-driven clinical insights, and secure, interoperable data flows. Whether you need compliance tools, shared savings tracking, or a care coordination engine, we align it with your quality metrics, reimbursement goals, and care delivery model.
Ready to Improve Outcomes with Custom Value-Based Solutions?
We design and build custom software for value-based healthcare, built around your data, workflows, and objectives. Whether you need to unify data, support attribution, or track performance across contracts—we’re here to build what works.
CMS LEAD Model Explained: Strategy, Risk & Readiness Checklist
RPM Impact Report: Reducing Nurse Burden & Attrition
The Clinical Impact Report: Precision Remote Patient Monitoring
Virtual Nursing Software Development: Building High-Availability Patient Monitoring for 2026
Checklist for Healthcare Organizations in 2026: Preparing for Value-Based Care
Patient Engagement Solutions for Hospitals: Custom Software to Accelerate Value-Based Care
Stay in the loop with everything you need to know.